Gut-Brain Axis: Do You Take Your Gut Feeling Seriously?

If you have a bad gut-feeling more frequently than you’d like to, you may have a gut-brain axis issue. Does this scenario sound familiar?
You feel down one day. It happens. It continues to another day. That’s still fine. You seem to be having a rough week.
On a second thought, has it been two weeks already? You start to feel irritable and you feel stressed most of the time.
Do you take your bad gut feeling seriously at that point? You should.
Psychologists say that if you feel helpless, hopeless or you don’t feel like doing what you like doing best – those are all signs of depression.
Causes of depression and anxiety are various, and it is always best to treat the root cause of these issues, whenever possible.
On the other hand, resolving the issues that cause your bad mood is a long and often complicated process. You need to start doing something right now to soothe the symptoms.
One of the physiological reasons you feel down can be low levels of serotonin, leptin, and ghrelin. This is rarely the only reason for feeling blue, but it is an important factor.
Your body is a complex machinery with all the organs and systems of organs working in synergy. So, would it really come as a surprise to you that your gut has a lot to do with your mood?
After all, don’t we all have “gut feelings” or experience “gut-wrenching moments”? Your gut is connected to your brain and plays an important role in the way you process your emotions.
This is called the gut-brain axis and it is a new, emerging idea that has been a topic of a lot of red light therapy research in recent years.
In other words, if you make sure your gut is nice and healthy, it can help you with your mood, anxieties, and depression.
Let’s dive deeper and try to answer some of the most common questions about the gut-brain axis.
How Does the Gut-Brain Axis Work?
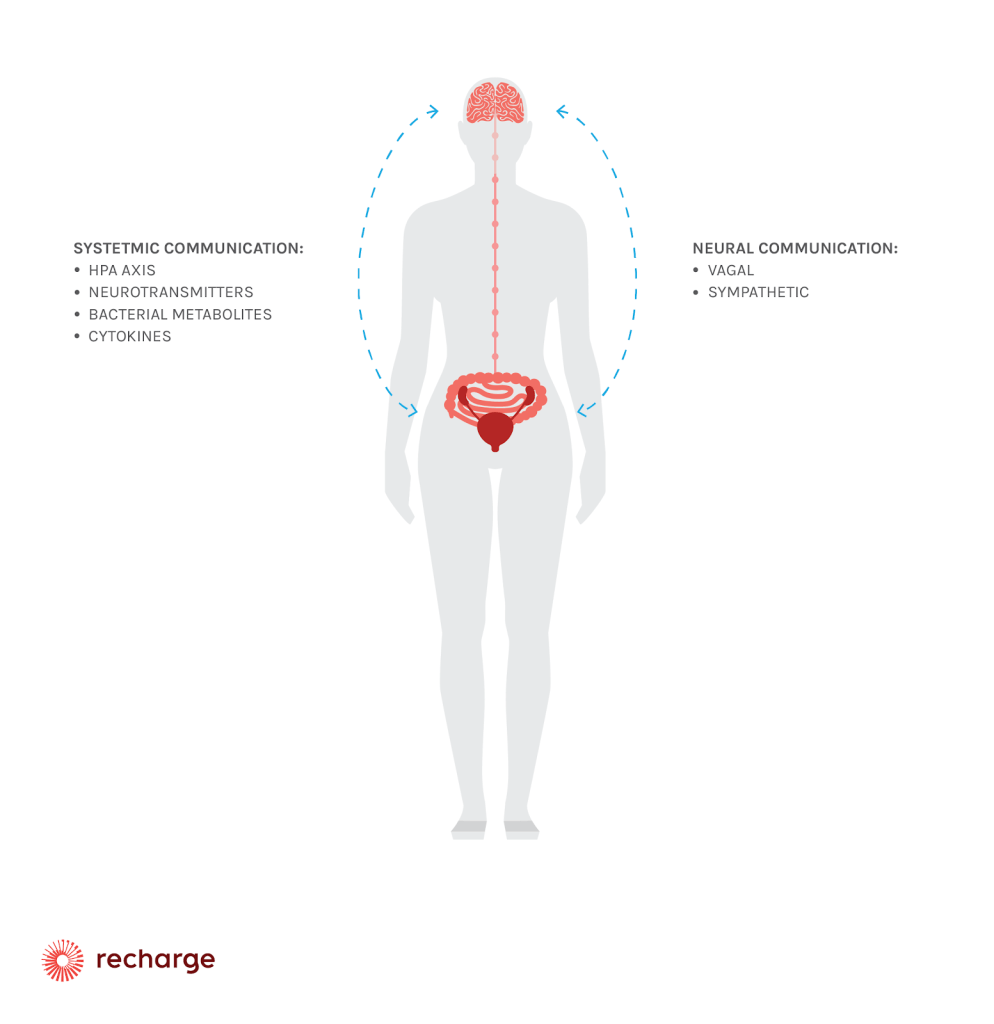
The connection between the gut and the brain (central nervous system, CNS) goes through two pathways points. The CNS has a sympathetic and parasympathetic system. Both of these communicate with the gastrointestinal system.
Another pathway is the direct connection between the central nervous system and the enteric nervous system (ENS). ENS is a separate nervous system that regulates the work of the gastro-enteric system.
Now, the gut is populated with trillions of microscopic organisms. All of those organisms together are called the microbiome.
Gut flora produces different types of molecules. Some of them cause reactions in neurons. Those are usually hormones, like melatonin or serotonin, but others, as well.
Those neuroactive molecules communicate with the central nervous system and cause different reactions.
For example, when you smell freshly baked cookies, your stomach starts growling. Your central nervous system detected the smell, associated it with the amazing taste of the cookies, and the gastro-enteric system prepares for a delicious treat.
This goes the other way around, as well. For example, if you are in stressful situations for prolonged periods of time, this will influence your gut flora. This happens via HPA connection, but also through the vagus nerve.
Can Gut Bacteria Cause Anxiety?
Gut bacteria can cause anxiety. Everybody knows about the “anxious stomach.” Increased stress levels can cause heartburn, nausea, bloating and worsen IBS symptoms.
Gut flora can also change the levels of cytokines. Cytokines regulate the states of anxiety and alarm in our brains. Therefore, if the gut flora influences their levels, it consequently affects your anxiety levels.
The levels of leptin (which acts both as cytokine and hormone) and ghrelin influence the levels of anxiety you experience.
Leptin is associated with motivation and anxiety in correlation to our basic “hunter” instinct. Low levels will increase anxiety. Ghrelin operates in a similar way.
Gut bacteria can regulate levels of these hormones and cytokines, making the gut-brain axis partly responsible for increased anxiety.
How Do You Heal the Gut-Brain Axis?
Choose Your Probiotics Wisely
Probiotics are quite efficient when it comes to regulating your gut bacteria. But not all of them will influence precisely the bacteria that affect your mood. Those probiotics that have these healing effects are called psychobiotics. Bifidobacterium infantis is one of the bacteria strains that can help alleviate anxiety. According to Science Daily, a significant number of studies proved this effect.
Mind Your Diet
Include omega-3 rich foods, fermented foods, and foods that contain tryptophan. Tryptophan turns into serotonin, so it is crucial in your diet. Tryptophan-rich foods are turkey, chicken, eggs, fish, pumpkin seed, and similar foods. Omega-3 is found in a lot of fish as well as in walnuts, while fermented foods include sauerkraut, kefir, tempeh, kombucha, and the like.
Find Your Calm with Yoga and Meditation
Yoga and meditation are excellent ways to cope with daily stress. Stressors will trigger biochemical reactions that will damage the gut bacteria balance. This imbalance will cause anxiety and depression. It is a vicious circle that needs to be broken by appropriate dealing with stressors.
Use Red Light Therapy for Best Results
The microbiome reacts to light. It responds by growing, migration and other processes. This means that by influencing the life of the microbiome, you directly influence the secretion of hormones and neurotransmitters.
Red light therapy is a direct and efficient way to help regulate and strengthen your gut-brain axis. Now, it is possible to do it at home with your portable device in just 10 minutes a day.
The gut-brain axis has been researched increasingly for the past couple of years.
This research will continue, especially the human trials, because there are indications that it can help bring us a step closer to solving Alzheimer’s and other neurological disorders.
Your health and well-being are influenced by your gut-brain axis. It affects your quality of life. So, take your bad mood seriously and do your best to elevate it.
